Faced with a problem such as varicose veins in the lower extremities, the patient should not hesitate to consult a doctor and start treatment. An experienced specialist will conduct a thorough examination and draw conclusions about which therapy tactics are best suited: conservative or surgical treatment. If, for some reason, the medications do not have the desired effect on the patient's blood vessels, doctors prescribe a surgical intervention, which can already help unconditionally.
Indications and if surgery is needed
Surgery to remove varicose veins is a radical approach in the treatment of pathological vessels, so the indications for it will be appropriate.

The operation will be justified in the following cases:
- total varicose veins of the lower extremities, which are visible to the naked eye;
- constant severe swelling of the legs, discomfort, pain, and a feeling of heaviness in the legs or elsewhere, depends on the location of the pathological process;
- a direct threat that varicose veins in a particular part of the body will be complicated by a more dangerous disease (eg, thrombophlebitis, trophic ulcer, or pulmonary embolism).
In a direct conversation with the doctor, he will be able to know if the operation is worth doing and also talk about the types of surgical interventions in general.
Contraindications for the surgical treatment of varicose veins
Despite the strong indications, there are many cases in which surgery to remove varicose veins in the legs cannot be performed. For example, if a patient has the last stages of varicose veins, surgical treatment will not always be possible. In these cases, doctors focus on drugs but cannot help enough.
A number of other mandatory contraindications:
- the presence of skin diseases at the affected vein site, eg eczema, pyoderma, dermatitis, etc.
- serious diseases of the cardiovascular system - hypertension, coronary artery disease, heart failure;
- acute inflammatory process within the vessel (phlebitis);
- thrombosis or previously transferred pulmonary embolism;
- active process of atherosclerosis obliteration;
- advanced age;
- period of pregnancy.
The patient must remember that, in the case of using medication for other diseases, the attending physician must be informed.
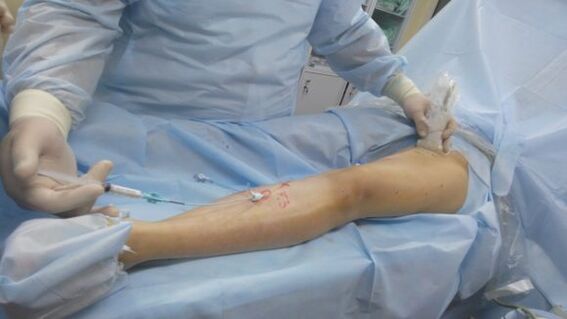
Sclerotherapy Technique
Sclerotherapy is a procedure whose principle is to inject a special substance into the affected vessel, causing more contraction and overgrowth of the vessel. The main advantage of this method is that the procedure does not require incisions or surgical access.
The essence of the procedure is as follows: with the aid of a syringe, the doctor injects a sclerosing substance into the pathological vessel. During a stage of sclerotherapy, a specialist gives two to ten of these injections. The effect does not appear at the same time - it usually takes 2 to 8 weeks and several sessions of such a procedure. Under the action of the sclerosant, the vein gradually narrows and then overgrows and disappears.
There are two types of manipulation:
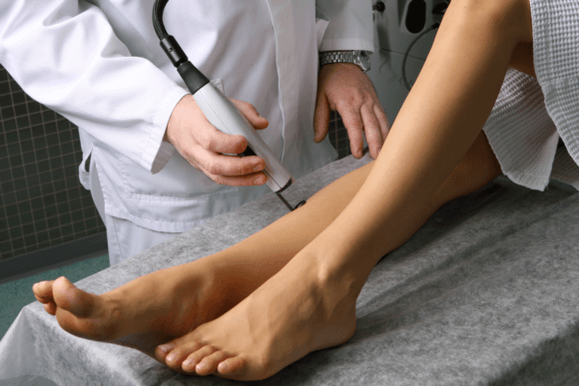
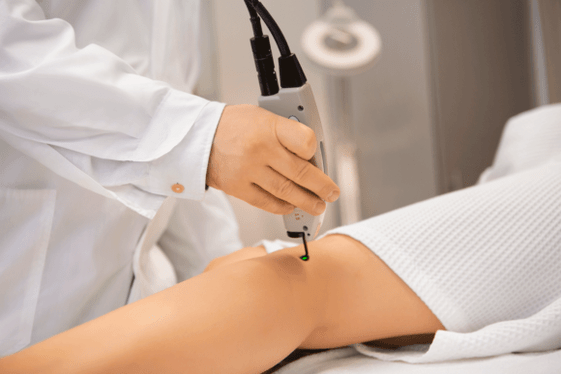
laser coagulation
Laser surgery for varicose veins is by far the most popular. This is because the procedure itself is performed under local anesthesia, does not require large incisions and tissue trauma, and has an immediate effect.
The vascular surgeon must tell in detail how the operation is performed, but in general its essence lies in introducing a special laser light guide into the diseased vessel. A laser beam, which has its own wavelength, passes through this device and acts on the walls of varicose vessels. Under its action, the vessel clots and clogs.
This technique will be justified if the patient has varicose veins in the leg or groin region. In addition, laser coagulation will act more effectively in large vessels, which is why the use of this technique in cases of injury to small veins is unjustified.
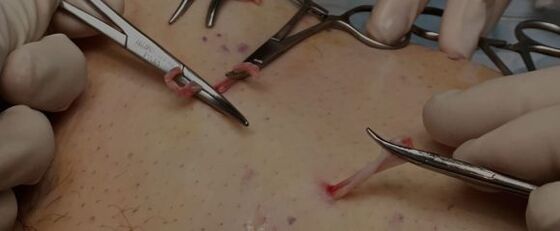
vein ligation
Vascular ligation is a more radical operation for varicose veins in the legs, requiring a large incision and direct surgical access.
The operation is performed on the legs more often than on the vessels in the pelvic region. The saphenous vein ligation technique will be effective. The vascular surgeon accesses the indicated vessel at the point where the saphenous vein and the femoral vein join. Then, the surgeon performs the bandage with special threads.
In women, pelvic vein surgery can be performed. In this case, the ovarian vein is accessed and ligated.
Removal of dilated vessels
The most common and proven method of surgery is phlebectomy. Doctors do it almost every day, and it's cheaper than laser coagulation or sclerotherapy. This operation for varicose veins is performed under general anesthesia or with epidural anesthesia.

To remove the dilated vessel, the surgeon needs an incision of only 0. 5-1 cm in length, having opened access to the area with varicose veins, the surgeon connects the vessel, crosses it and removes it.
As a subspecies of this intervention, miniphlebectomy is differentiated. It differs from conventional phlebectomy in that the surgeon needs punctures rather than incisions to access the vessel. This operation is effective in affecting small superficial vessels. Its main advantage is that it leaves no traces and aesthetic defects.
stripping
Stripping is one of the subtypes of phlebectomy, during which a special probe is used to remove a vein. As with simple varicose vein removal, the surgeon makes an incision in the saphenous vein and accesses the vessel. Then the doctor makes another incision - in the middle or lower part of the leg.
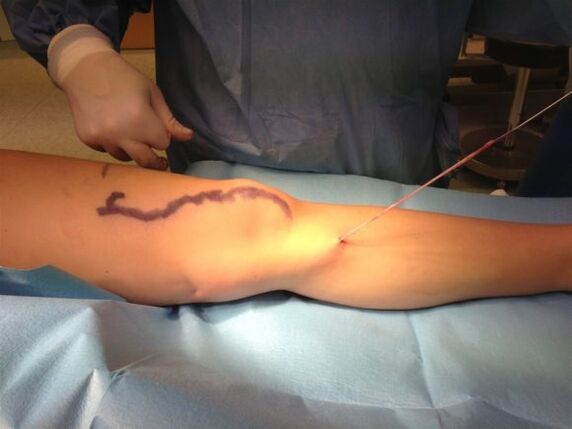
Through the superior access to the great saphenous vein, a special probe is introduced - an extraction probe. The surgeon pre-dresses the mouth of adjacent veins. The probe is passed along the entire length of the vessel to the inferior incision, after which it is used to remove the vein.
On removal, several types of manipulation are also distinguished:
Consequences of surgery and rehabilitation
Having varicose veins, the operation can have the opposite effect and cause various complications. They must be separated by the type of intervention performed:

For all surgical treatment methods, there is a common complication - thrombosis. This is a dangerous process, but the chance of it occurring as a result of any operation is very low.
To avoid the aforementioned complications and to shorten your rehabilitation period as much as possible, you should follow the post-operative health and blood vessel care recommendations.
Subject to post-operative rules, symptoms disappear within a few days.
There are a number of pros and cons that experts recommend following:
- Immediately after the end of the operation and for the first week after, it is necessary to wear special compression briefs - it can be in the form of pantyhose, pantyhose, stockings, and for this you can also use a common elastic bandage.
- Eliminate bad habits - alcohol consumption, smoking, drug use.
- Avoid baths and saunas, in addition to taking very hot baths.
- In the place where the operation was performed, it is not possible to carry out any cosmetic procedure and apply various cosmetics.
- Avoid strenuous physical activity. In case the patient practices any kind of sport (especially hard) before the treatment, after the operation, heavy loads should be forgotten for at least 5 to 8 weeks. In the future, you should see your doctor if you can continue with intensive sports.
- Do daily prophylactic exercises lasting no more than 15-30 minutes.
- Follow the phlebologist's prescription for taking medications - take regular prophylactic anticoagulants, phlebotonics, nonsteroidal anti-inflammatory drugs, thrombolytics and other medications.
In general, all of these operations have good reviews from doctors and patients. Which treatment approach is suitable for a particular patient needs to be decided only with the responsible physician.























